Troy Shantz
Warm afternoon sunshine washes into a shared hospital room at Bluewater Health, where a couple occupies adjacent beds.
Both have COVID-19.
It is now clear to hospital staff the woman is recovering. Her husband’s prognosis is much less certain.
Throughout the night they have held each other’s hand, says one of the nursing staff caring for them.
“I put their beds together. It’s quite lovely,” she adds.
“It makes me feel like a good nurse.”
Bluewater Health has established a specialized COVID-19 unit in what was formerly the rehabilitation ward. It has space for up to 40 beds.
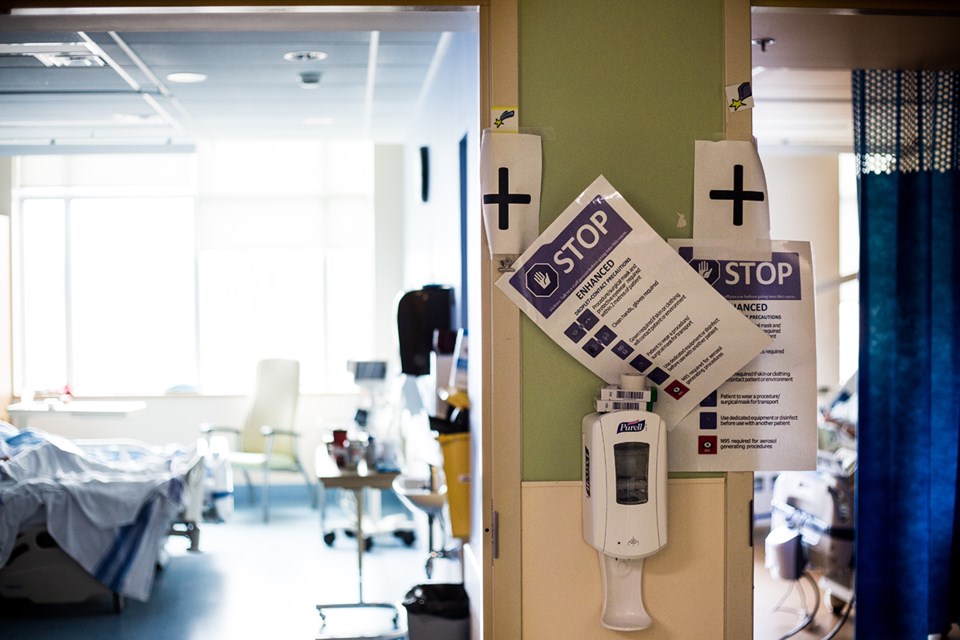
Along one hallway are rooms with patients presumed to have contracted the virus, and in another are confirmed cases, their door frames marked with a bold “+” for positive.
As of Monday, the hospital was treating 29 patients confirmed with the novel coronavirus, as well as another 12 presumed infected and awaiting test results.
If needed, dozens of additional rooms can be mobilized throughout the hospital, which is currently operating at about 60% capacity, officials say.
Teams of registered nurses, registered practical nurses and personal support workers assist the patients in a ratio of 1:4. Each is covered in protective gowns, gloves and masks.
Social work, physiotherapy and occupational therapy professionals are also part of the team,” explains Laurie Zimmer, the hospital's vice-president of operations.
“Some of these nurses haven’t worked together before,” she said.
“We had volunteers come and say, ‘Yes, I want to work in the (COVID) unit, to help these patients.’ We’re very proud and very supportive of the staff.”
The sickest patients are treated in the intensive care unit, separate from the COVID unit, she said.
Images of overwhelmed hospitals in China, Italy, Spain and New York have dominated the news lately, but here, on this day, things are organized and orderly.

Health-care workers move swiftly from room to room, while environmental services staff busily wipe down every surface in sight.
“It’s a busy unit. You have a lot of people admitted and a lot of people discharged,” said Zimmer.
“Actually, people recover a lot nicer at home. They’re in their own surroundings; they’re able to get moving. If we can get patients home we aim to do that.”
As of the weekend, 16 patients had been discharged from hospital, she added.
Downstairs, screeners in the emergency room immediately greet new arrivals with a simple question: do you have symptoms of COVID-19?
“They’re asked the screening questions around any fever, any travel in the last 14 days,” said Zimmer.
“They’re also given a mask if they have any sort of respiratory symptoms.”
It’s Monday, and the ER is quiet.
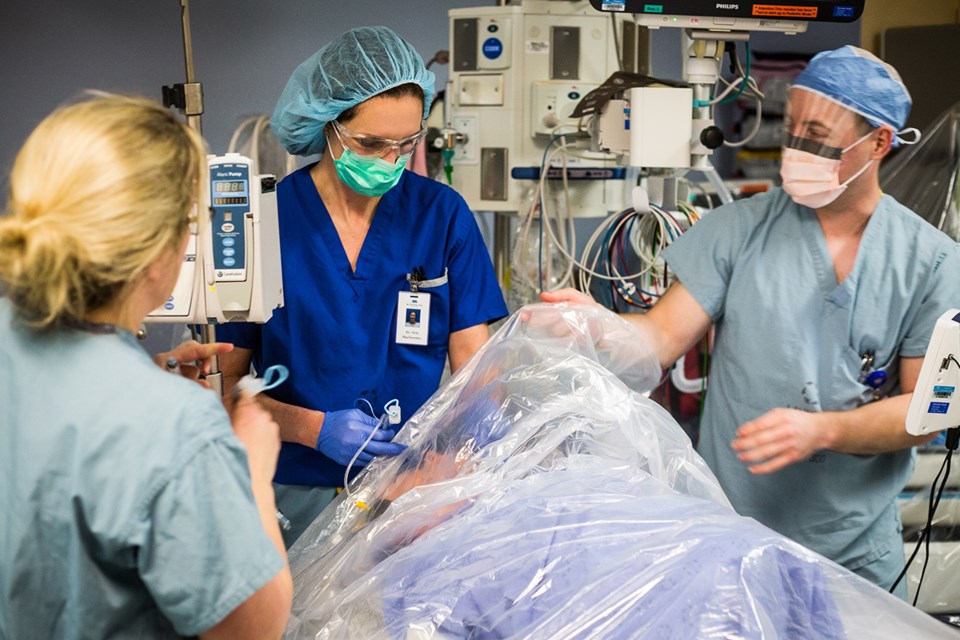
In a nearby examination room, doctors are practicing intubation on a medical dummy, its torso draped with a plastic sheet.
They’re working on reducing the spread of infectious droplets patients can emit during procedures, explains Dr. Orla MacSweeney.
“It’s a debate,” she says, guiding a tube through the dummy’s airway. “What we really want is to increase the likelihood of us getting the airway successfully (open) without contaminating the room.”
The doctors eventually conclude the process would cause too much patient anxiety.
Being infected with a virus that has killed eight people in Sarnia-Lambton 80,000 worldwide is frightening enough.